When people hear the word kyphosis, they often picture an exaggerated hunch—something dramatic, obvious, and usually associated with aging. In practice, it’s far more subtle than that, and far more common. I see it in people who exercise regularly, people who sit at desks all day, teenagers, retirees, and just about everyone in between.
So, what is kyphosis, really? And more importantly, why does it matter long before it becomes severe or painful?
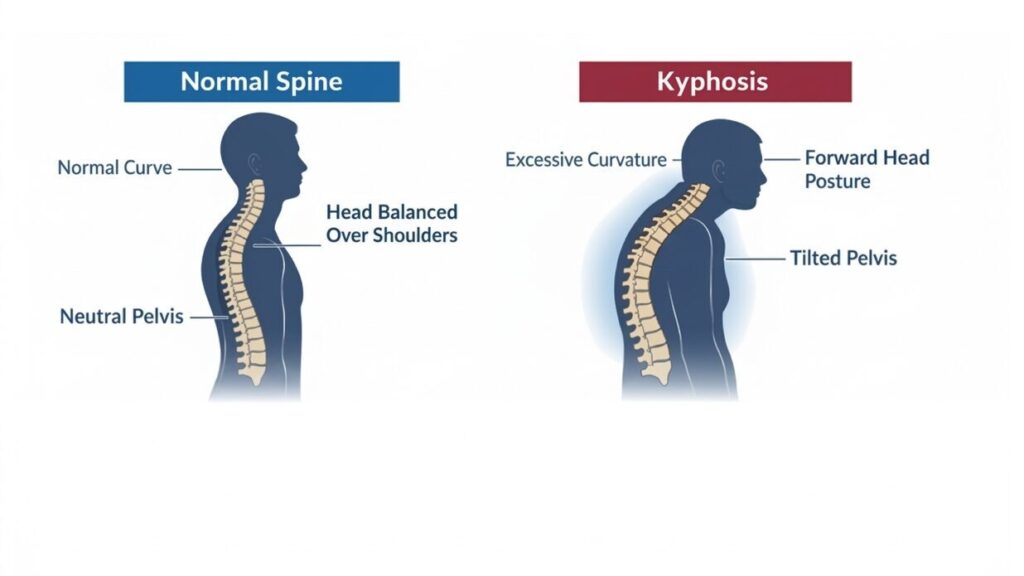
Kyphosis refers to an increased forward curvature of the thoracic spine—the mid-back. A certain amount of curvature there is normal and healthy. The problem arises when that curve becomes excessive or progressive, often without the person realizing it’s happening.
Most people don’t wake up one morning with kyphosis. It develops quietly, over years, as the body adapts to how it’s used.
What do you understand by kyphosis?
Clinically, kyphosis is a structural or functional increase in the thoracic curve beyond what’s considered normal for that individual. That distinction—structural versus functional—matters more than most people realize.
A functional kyphosis is flexible. When someone lies down, extends their spine, or consciously corrects their posture, the curve improves. Structural kyphosis is different. The spine itself has adapted. Ligaments have lengthened, discs have remodeled, and vertebral alignment has changed. At that point, simply “standing up straighter” doesn’t last.
This is often where confusion sets in. People assume posture problems are just habits. Sometimes they are. Often, they’ve already crossed into something deeper.
What causes kyphosis?
When patients ask me what causes kyphosis, I usually pause before answering. Not because it’s complicated, but because the real answer isn’t a single thing.
Kyphosis tends to develop from cumulative stress rather than isolated events. Long hours of forward-focused work. Screens held low and close. Repetitive tasks that keep the shoulders rounded and the head drifting forward. Over time, the body adapts to those positions because it’s efficient, not because it’s optimal.
There are also developmental and structural contributors—growth spurts, past injuries, degenerative disc changes, compression fractures, or conditions like Scheuermann’s disease. But even in those cases, posture and mechanical loading influence how the curve progresses.
One pattern I’ve noticed over the years is this: people often feel fine while kyphosis is developing. The discomfort shows up later, once the spine has already adapted. By then, they’re treating symptoms of a structural issue, not the issue itself.
Why kyphosis affects more than posture
It’s tempting to think of kyphosis as a cosmetic problem. Something about appearance. In reality, posture is more like a window than a mirror—it reflects what’s happening underneath.
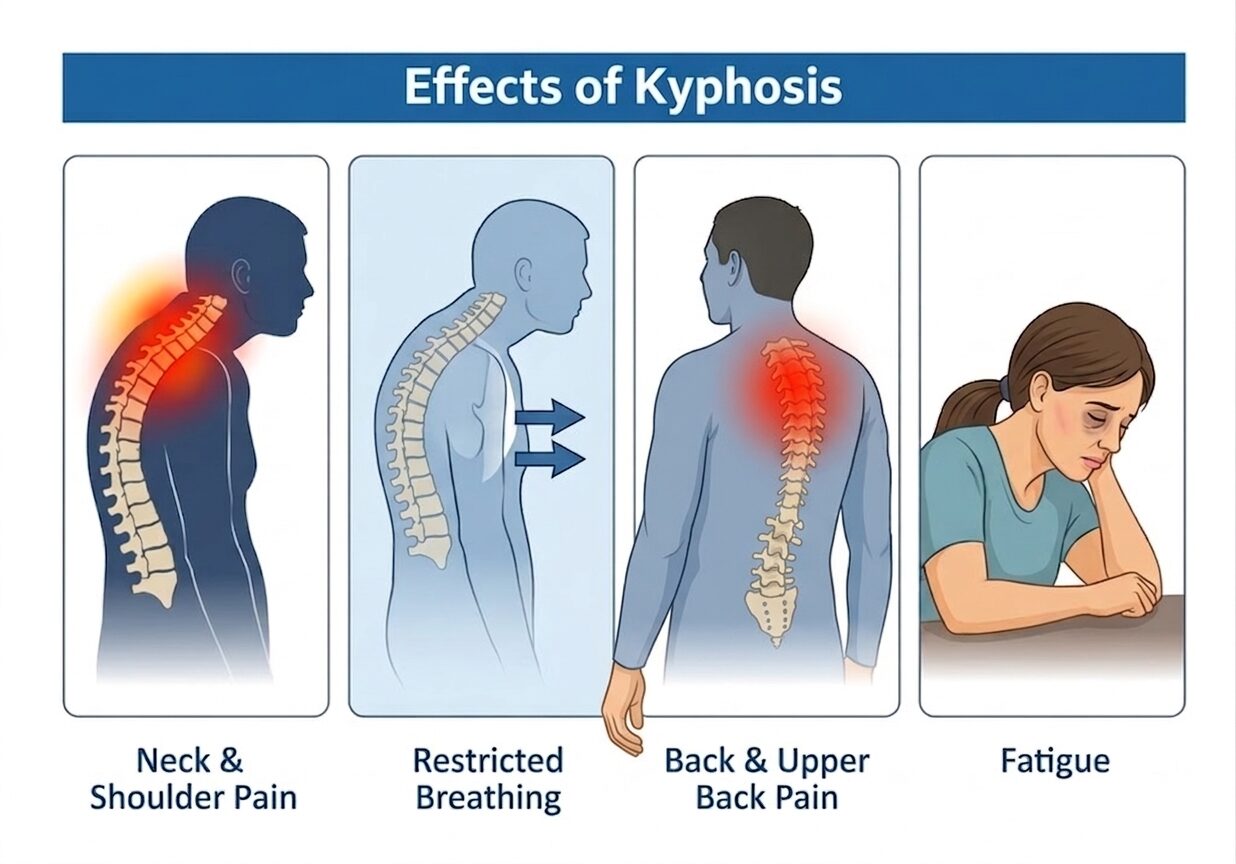
As the thoracic curve increases, the rib cage changes position. Shoulder mechanics shift. Breathing patterns subtly adapt. The head often moves forward to compensate, increasing strain on the neck. None of this happens dramatically, but the cumulative effect matters.
I’ve seen patients who came in for neck tension, shoulder pain, or even unexplained fatigue, only to discover that their thoracic posture was driving much of what they were experiencing. The body is excellent at compensating—until it isn’t.
Posture exercises for kyphosis: helpful, but not sufficient alone
There’s no shortage of posture exercises for kyphosis online. Some are useful. Many are well-intentioned. A few are oversimplified.
Exercises that strengthen the mid-back, improve shoulder mobility, and encourage thoracic extension can absolutely help—especially in early or flexible cases. They can improve awareness, coordination, and short-term posture control.
In many cases, this forms just one part of a broader kyphosis treatment approach focused on correcting spinal alignment and addressing both muscular function and underlying spinal structure.
Where people get frustrated is when they do everything “right” and the posture still reverts. That’s usually not a motivation problem. It’s a structural one.
Exercises influence muscles. Kyphosis, once established, involves ligaments, discs, and joint positioning. Muscles can’t permanently override those tissues. This doesn’t mean exercise is pointless—it means it has to be paired with an understanding of structure and load.
In clinic, I often explain it this way: muscles are the steering wheel, but structure is the alignment of the tires. You can steer all you want, but if the alignment is off, the system keeps pulling back.
How to correct kyphosis posture problems?
When someone asks, how to correct kyphosis posture problems, the honest answer depends on the individual.
The first step is distinguishing between a posture that’s flexible versus one that’s adapted. That requires assessment, not guesswork. From there, correction usually involves a combination of targeted movement, external support or traction, and consistent mechanical input over time.
What doesn’t work well is relying on reminders, braces worn inconsistently, or exercises chosen at random. Posture doesn’t change because we tell it to. It changes because the nervous system and connective tissues receive a repeated, specific signal that a new position is safe and sustainable.
Some people respond quickly. Others need patience. In both cases, progress tends to be incremental, not dramatic—and that’s actually a good sign.
A quieter way of thinking about posture
One of the most helpful reframes I’ve found is this: posture isn’t something you hold. It’s something you become accustomed to.
Your body will always default to what feels normal. The goal isn’t perfection. It’s shifting what “normal” feels like.
When people understand that, they stop blaming themselves for not sitting up straight all day. They start asking better questions. And that’s usually when real change becomes possible.
Kyphosis isn’t a verdict. It’s information. A snapshot of how the body has adapted so far.
If you’re curious about your own posture, the most productive next step isn’t panic or aggressive correction. It’s learning—about your structure, your habits, and what your spine has been quietly responding to over the years. That kind of understanding tends to open doors rather than close them.
About the Author

Dr. David Shapiro, DC, CEO of Complete Spine Solutions
Dr. Shapiro is a graduate of Life University School of Chiropractic (1993) with more than 4,600 hours of postgraduate education. He is a licensed Doctor of Chiropractic who has passed three national board examinations as well as the Georgia state board examination. He is also certified in therapeutic modalities and is an Advanced Certified practitioner of Chiropractic BioPhysics®.
He focuses on identifying and correcting structural spinal changes such as kyphosis, helping patients address the underlying mechanics—not just the symptoms. His approach centers on restoring proper spinal alignment over time, improving posture, reducing strain on the body, and supporting long-term function without reliance on medication.
If you’re concerned about forward posture or developing kyphosis, a proper assessment is the first step. Book a free consultation or call us at (770) 938-4606 to get started.






