
Fibromyalgia is one of those diagnoses that tends to raise more questions than it answers. Many people arrive at it after years of symptoms, multiple opinions, and a growing sense that something is wrong—but nothing clearly shows up on scans or lab work. That disconnect can be frustrating, and for some, even invalidating.
At its core, fibromyalgia is characterized by widespread pain, fatigue, sleep disturbance, and heightened sensitivity to physical and emotional stress. But those words only skim the surface. To really understand fibromyalgia, it helps to look less at individual symptoms and more at patterns—especially patterns involving how the nervous system processes information over time.
Who Is Affected by Fibromyalgia?

When people ask who is affected by fibromyalgia, the most common answer is “women between 30 and 60.” Statistically, that’s true. Women are diagnosed far more often than men, and symptoms frequently emerge in midlife.
But statistics don’t tell the whole story.
In clinical practice, fibromyalgia often shows up in people who have lived for years under sustained stress—sometimes physical, sometimes emotional, often both. That stress might include prior injuries, repetitive strain, long-term poor sleep, autoimmune conditions, chronic inflammation, or even prolonged periods of caregiving or high responsibility with little recovery.
Men get fibromyalgia too. They’re just less likely to be diagnosed. Children and adolescents can develop similar symptom patterns, though they’re often labeled differently. What ties these groups together isn’t age or gender so much as nervous system overload.
That’s an important distinction.
Fibromyalgia Symptoms: More Than “Just Pain”
Fibromyalgia pain is typically described as widespread, aching, burning, or deep. But pain is rarely the only complaint. Many people also report:
- Non-restorative sleep
- Persistent fatigue that doesn’t improve with rest
- Brain fog or difficulty concentrating
- Heightened sensitivity to touch, sound, light, or temperature
- Digestive issues
- Headaches or jaw tension
What’s striking is how these symptoms tend to cluster. They don’t behave like isolated problems. They behave like a system that’s lost its ability to regulate.
From a clinical perspective, that matters.
What Causes Fibromyalgia?
The short answer is that fibromyalgia doesn’t have a single cause. There’s no infection, injury, or deficiency you can point to and say, “That’s it.”
A more useful way to think about what causes fibromyalgia is to view it as a state of nervous system sensitization. Over time, the brain and spinal cord become more reactive to input. Signals that should be filtered or dampened are amplified instead.
Pain thresholds drop. Recovery slows. Stress tolerance narrows.
This doesn’t happen overnight. It’s usually the result of accumulated load—physical strain layered on top of emotional stress, layered on top of poor sleep or unresolved injury. Eventually, the system adapts by staying on high alert.
It’s not a weakness. It’s a survival strategy that’s gone on too long.
Why Standard Treatments Often Fall Short
Conventional treatment for fibromyalgia often focuses on symptom management: medications to dull pain, improve sleep, or stabilize mood. For some people, these provide partial relief. For many others, the benefits are modest and temporary.
That’s not because fibromyalgia is “untreatable.” It’s because the approach doesn’t always match the problem.
If the underlying issue is a sensitized nervous system, then treatments that only target chemistry—without addressing mechanical stress, movement patterns, or structural load—can miss key contributors. Pain may quiet briefly, but the system remains irritated.
In practice, this is why people often say, “Nothing really helped, but some things helped a little.”
A Different Lens: Structure, Load, and Neurological Input
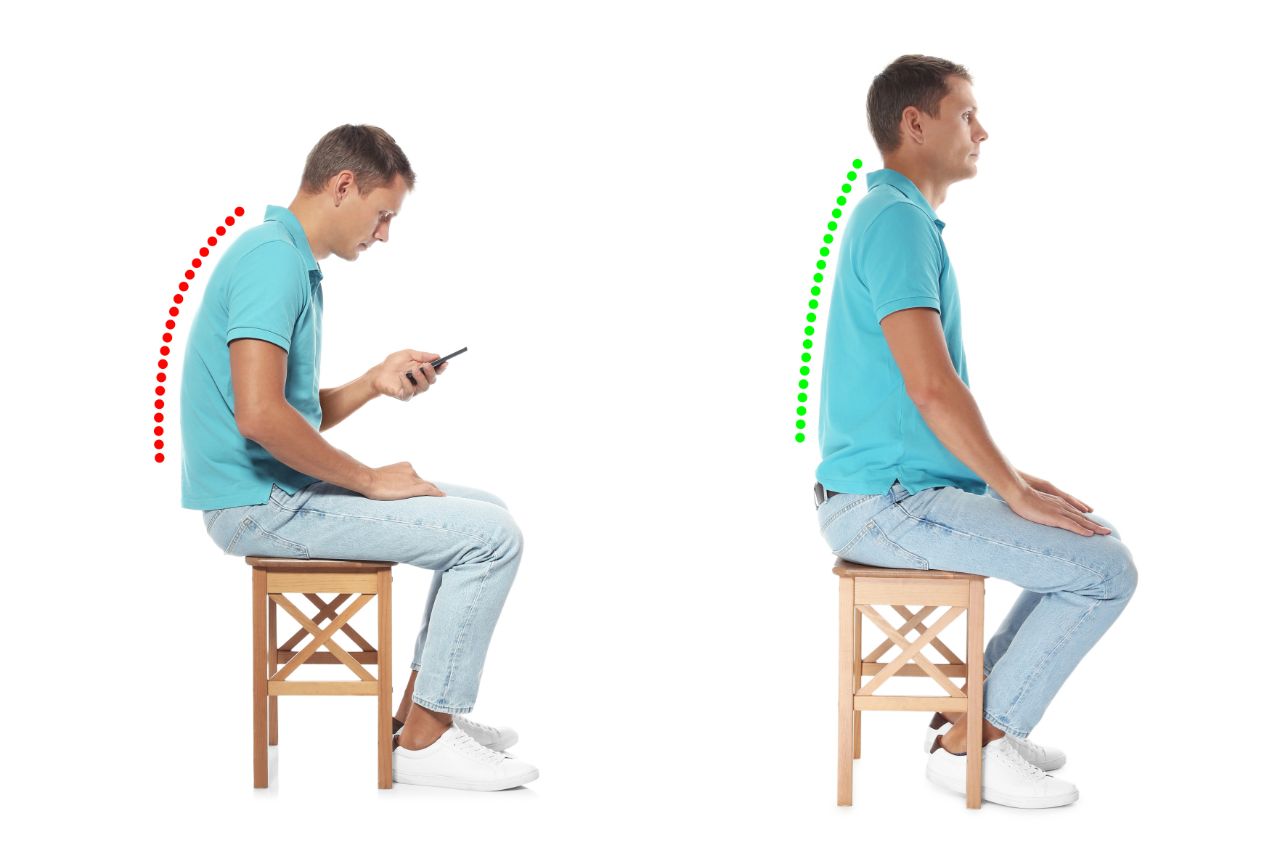
One of the quieter conversations in fibromyalgia care involves how the body is physically organized. The spine, posture, and movement patterns matter—not because fibromyalgia is a “spinal problem,” but because the nervous system lives inside a physical framework.
When that framework is under chronic strain—forward head posture, collapsed ribcage, reduced spinal motion—the nervous system receives constant mechanical stress signals. Over time, that input can reinforce sensitization.
This doesn’t show up on blood tests. It doesn’t always show up on MRIs. But it shows up in how people move, breathe, and recover.
Clinically, when those mechanical stresses are reduced and neurological input becomes more consistent and organized, many patients report changes that go beyond pain alone. Sleep improves. Fatigue lifts. Resilience returns, often gradually.
That’s not a quick fix. It’s a different trajectory.
Fibromyalgia Therapy and Treatment: Thinking Long-Term
Effective fibromyalgia therapy tends to work best when it respects complexity. That means moving away from the idea that one intervention should “fix” everything, and toward a model that reduces total system load over time.
Treatment for fibromyalgia often benefits from approaches that:
- Calm the nervous system rather than stimulate it
- Improve movement quality without overexertion
- Restore structural balance to reduce ongoing stress signals
- Respect pacing and recovery
Progress is rarely linear. There are good weeks and frustrating ones. But when care is oriented toward restoring regulation—not just suppressing symptoms—the gains tend to hold better.
Living With Fibromyalgia, Differently
One of the hardest parts of fibromyalgia isn’t the pain itself. It’s the uncertainty. People are often told their tests are normal, that they should “manage stress,” or that this is something they’ll just have to live with.
That framing doesn’t leave much room for hope—or understanding.
A more grounded perspective recognizes fibromyalgia as a real, embodied condition involving how the nervous system has adapted to long-term load. And adaptations, by definition, can change.
Not overnight. Not magically. But thoughtfully.
If you’re exploring fibromyalgia on your own, asking better questions is a good place to start. Questions about patterns, structure, recovery, and regulation—rather than just chasing the next symptom solution.
Sometimes clarity comes not from doing more, but from finally seeing the problem through a wider lens.
About the Author

Dr. David Shapiro, DC, CEO of Complete Spine Solutions
Dr. Shapiro is a graduate of Life University School of Chiropractic (1993) with more than 4,600 hours of postgraduate education. He is a licensed Doctor of Chiropractic who has passed three national board examinations as well as the Georgia state board examination. He is also certified in therapeutic modalities and is an Advanced Certified practitioner of Chiropractic BioPhysics®.
Dr. Shapiro focuses on correcting structural spinal changes while supporting the nervous system’s adaptation to long-term stress. His approach goes beyond symptom relief, helping patients with fibromyalgia improve posture and movement and reduce ongoing strain on the body.
If you’re experiencing persistent pain, fatigue, or fibromyalgia-related symptoms, a comprehensive assessment can help guide your next steps. Book a free consultation or call us at (770) 938-4606 to get started.






